Osteoarthritis (OA) is the most common form of arthritis. A chronic joint condition, cartilage gradually thins and the entire joint undergoes change that leads to pain, swelling, and loss of function. OA most often involves knees, hips, hands, and the spine. Risk rises with age, prior injury, excess body weight, and repetitive joint stress, impacting women more than men.
Symptoms usually develop slowly. People notice morning stiffness that eases with gentle movement, aching that worsens after activity or at day’s end, and intermittent swelling or warmth. Hands may develop bony enlargements at the finger joints; knees can feel unstable or “catch,” and hips often cause groin or buttock pain with walking or turning. Over time, flare–quiet cycles give way to more persistent discomfort and reduced range of motion that can limit work, caregiving, and recreation if not addressed early. (NIAMS)
Diagnosis is clinical, supported by imaging when needed. A clinician will review symptom patterns, examine joint line tenderness, swelling, crepitus, alignment, and gait, and consider other causes of pain such as inflammatory arthritis or tendon disorders. X-rays can show joint-space narrowing and bony spurs; MRI is reserved for selected cases to assess cartilage, bone marrow lesions, or meniscal pathology. Lab tests are typically normal in OA and are used primarily to rule out other conditions. (MedlinePlus)
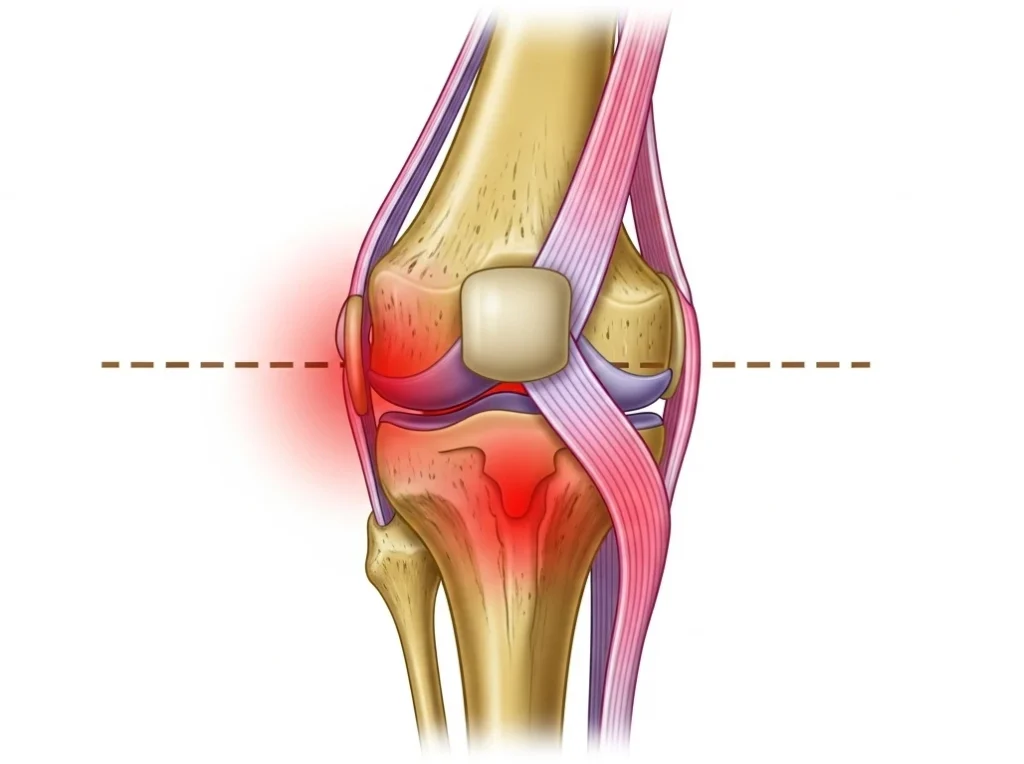
Treatment aims to reduce pain, preserve function, and slow disability with a stepwise plan tailored to the person and joint involved. The foundation is non-drug therapy: regular, joint-friendly exercise that builds strength and flexibility, weight reduction when indicated, physical therapy for gait and muscle balance, and assistive devices such as canes, braces, or shoe inserts to improve mechanics and reduce load across painful compartments. Even modest weight loss can meaningfully reduce knee load and pain, and structured self-management programs help people stay active and confident. (CDC)
Medications are added when symptoms persist. Topical NSAIDs (such as diclofenac gel) are a first choice for hand and knee OA because they provide local relief with lower systemic exposure; oral NSAIDs can be effective for flares if cardiovascular, kidney, and gastrointestinal risks are considered. Acetaminophen may help mild pain but is often less effective than NSAIDs. For some individuals, agents like duloxetine can help chronic musculoskeletal pain, and capsaicin cream may offer additional topical relief for hands or knees. Decisions weigh benefits against side effects and other health conditions.
Injections are an option for targeted relief. Intra-articular corticosteroids can reduce inflammation and pain for weeks to months, especially during exacerbations; frequency is limited to avoid cartilage harm. Hyaluronic acid injections are used for some knees, though benefits are variable and patient selection matters. These procedures complement—not replace—exercise and mechanical offloading, and they are considered when daily activities are hindered despite optimized basics.
Surgery is reserved for significant pain, deformity, or functional loss after conservative care. Arthroplasty (joint replacement) of the hip or knee reliably relieves pain and improves mobility for advanced OA, while hand procedures and osteotomies may help carefully selected joints or alignments. Pre-operative strengthening, weight management, and planning for home support improve recovery, and most people resume everyday activities with less pain after rehabilitation.
Living with OA means managing the whole person, not just the joint. Regular activity—walking, cycling, water exercise, tai chi—reduces pain perception and improves balance and mood. Sleep, stress management, and treatment of coexisting conditions like diabetes and depression influence outcomes, as does quitting smoking. Vaccinations and fall-prevention strategies protect independence, and periodic follow-up allows the care plan to adjust as needs change across seasons and years.
The outlook has improved as care has become more comprehensive. Many people maintain active, fulfilling lives by combining exercise, weight control, symptom-guided medications, and selective procedures when necessary. Early recognition and a tailored plan—built with a clinician who understands your goals—offer the best chance to keep you moving, protect the joints you have, and time interventions wisely if you ever need more.
Clarity-Spot is for informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on Clarity-Spot.
